International Day of Women and Girls in Science is marked every 11th February as a global celebration of the accomplishments of women in science and to encourage young girls to consider a future career in STEM fields.
Francisca Mora, Senior Clinical Embryologist at Aria, along with clinical embryologist Summer Sorensen and embryologist Kim Hill, share their knowledge and unique insights into the fascinating field of embryology.
What led you to pursue a career in embryology?
“I’ve always known I’d work at something related to obstetrics. My parents say that I was always drawing pregnant women and babies when I was a child, maybe that was a tell?” Francisca reveals.
For Summer, the fascination with fertility started at High School when she attended a Science and Technology Forum and the keynote speaker explained all about the wonderful world of IVF. Kim undertook a Medical Physiology post-grad degree in South Africa that allowed her to be a part of the Reproductive Research Group, where her focus was on male fertility and nutrition.
What education / training did you go through to become an embryologist?
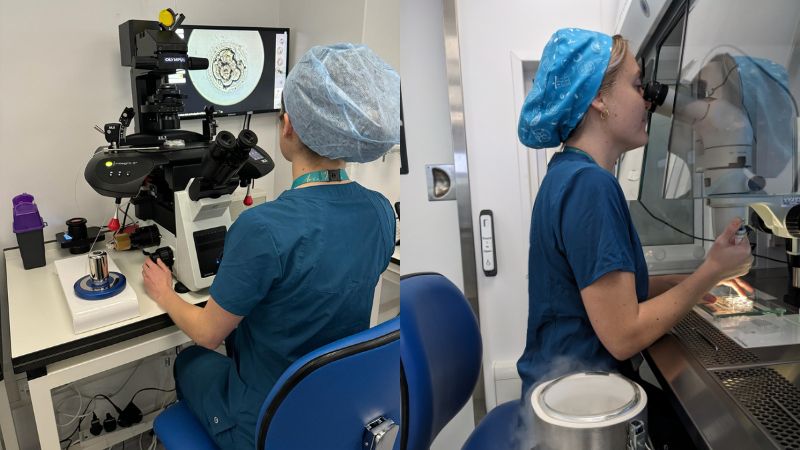
Before working in IVF in the UK, all three of our embryologists first studied in their home countries.
Summer completed a Bachelor of Biomedical Science (majoring in Reproduction, Genetics and Development) before completing a Bachelor of Biomedical Science with Honours, both at the University of Otago in New Zealand. She then completed her Masters of Clinical Embryology at Monash University in Melbourne, Australia.
Her first job was a trainee position at Fertility Associates in Auckland, New Zealand where she learnt all the necessary skills of being an embryologist.
Kim completed a BSc in Human Life Sciences & Psychology at Stellenbosch University in South Africa, then completed a Master’s Degree in Clinical Embryology at the University of Dundee.
After completing her MSc, she worked as a lab technician before advancing to a trainee embryologist. “I had in-house training, in both private and NHS settings, up to biopsy practitioner, before applying for professional registration. In this time, I also gained accreditation by the European Society of Human Reproduction and Embryology (ESHRE) as a Clinical Embryologist.”
Francisca holds a BSc and MSc Biochemistry from leading Portuguese universities. “I’ve also conducted my master’s thesis on the topic of male infertility. However, I’d say that my training didn’t start until I set foot in an IVF clinic and since then it has been an ever-growing experience, we are continuously learning! Since I’ve moved to the UK, I’ve learnt a great deal through colleagues, workshops, talks and the HFEA. Furthermore, acquiring my professional registration, has also been a key moment in my training.”
How do you stay current with the latest research and advancements in embryology?
“Aria Fertility supports an environment dedicated to improving outcomes through innovations in technology,” Kim explains. “Staying current with scientific advancements and professional recommendations enables us to provide state-of-the-art patient care.
This can come through a variety of sources. “Reading the latest scientific journal articles, attending conferences, LinkedIn, workshops, these are all useful,” Summer adds.
“Moreover, one of the most practical ways is to keep an eye on the embryology hubs that exist online; in that sense, social media has been very helpful in diffusing the latest developments,” Francisca points out.
What is the process or protocol that has most surprised you in terms of development and research?
“I’d probably say that trophectoderm biopsy, used for genetic testing (PGT), has been the process that surprised me the most,” Francisca explains. “Not only because I had not seen it before until I moved to the UK but was well for the level of detail and technical skill that it entails. It’s also a protocol that has evolved quite a lot in the last years, especially the technique used at the genetics lab to detect the abnormalities.”
How have recent advancements in embryology, like genetic screening, affected your work?

Both Kim and Francisca feel that genetic screening has greatly expanded their skill set and how they can guide patients through their treatment. “I became an embryo biopsy practitioner about a year and a half ago so the whole process is still very exciting to me,” Kim explains. “It is a valuable skill set to have, and unique as not all clinics provide genetic testing to their patients.”
“On one hand, such processes have made my work more challenging, in a positive way, since it has raised the bar for my skills and knowledge,” Francisca agrees, “and on the other hand, it has made it easier to guide patients on their treatment, as genetic screening can provide crucial answers.”
Summer feels that the greater awareness of egg freezing has had a huge impact on the fertility sector. “While egg freezing isn’t necessarily a new technology, I have really enjoyed the rise in awareness of this technology in the public space, and how more and more women are thinking about and planning their reproductive futures.”
What are some of the most exciting future possibilities in the field of embryology?
All three embryologists agree that AI will be the big focus in IVF. “It is very interesting to see what avenues are being explored and how this may impact our day-to-day procedures and the positive influence on our patients’ goals,” Summer explains.
“However, there will always be a need for a human embryologist on the other end of the line to support patients through the emotional impact and big decisions involved in IVF,” adds Kim.
Another possibility is creating eggs and sperm from stem cells. “I feel the possibility of creating gametes from other cells of one’s body could be a reality at some point, and this could bring hope to oncology patients,” Francisca expands.
Beyond the lab, what role does communication play in your job?
“As a clinic, we feel communication with our patients is one of the most important aspects of their treatment, for them to understand the process, the risks and to ask any questions they may have,” Summer explains.
“Patient interaction is my favourite part of the job,” Kim agrees. “I love explaining what goes on so that patients don’t feel the lab is a ‘black box’ of unknowns, and the decisions can be made together.”
Communication between team members is also vital. “Considering we all work under a lot of pressure and in a confined space, it’s super important to communicate effectively with colleagues to ensure that everything goes as smooth as possible,” Francisca explains.
“This helps when liaising with patients who can tell there is really good communication amongst the lab and greater team,” Kim agrees.
Is there a ‘typical’ workday at Aria Fertility?
“I’d say that each day can be quite different, as there are no equal cases, however there is a main structure that is followed every day,” Francisca explains.
The mornings tend to be busy with fertilisation checks, thawing embryos for embryo transfers later in the day, egg collections, embryo grading and sperm preparation. The afternoons are typically filled with inseminations (either conventional IVF or ICSI -sperm injection into the egg), embryos transfers, preparing for the next day and diagnostic sperm analyses.
What is the hardest part of your job?
Our embryologists all agree on what is the hardest part of their job.
“It’s without a doubt having to give bad news to the patients or to see that their treatment wasn’t successful,” Francisca explains. “Each failed fertilisation, negative pregnancy test, each pregnancy loss really takes a toll on all of us at Aria Fertility.”
“It never gets easier to tell a patient that is hasn’t worked this time,” Summer agrees.
“We want every outcome to be a success, but unfortunately science is not that robust yet, and this is a huge drive to keep developing the research behind IVF so we can better the chances of success,” Kim resolves.
What is your favourite part of your job?
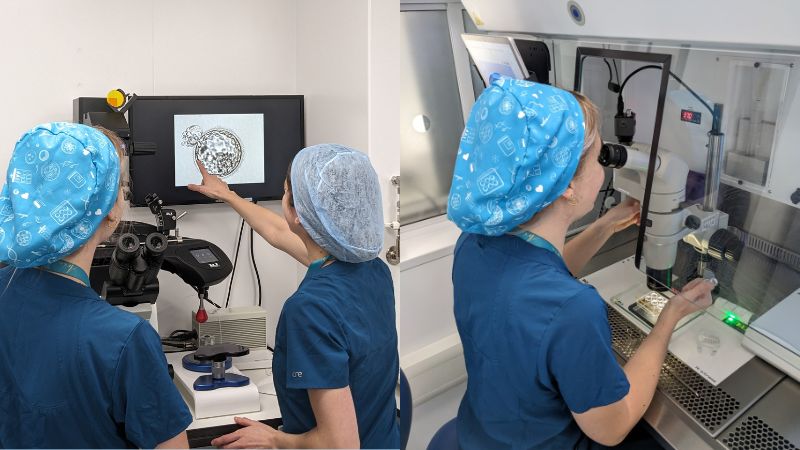
“My favourite lab procedures are egg collections and ICSI. But, overall, my favourite parts are the conversations with patients, and ultimately having a helping hand in our patients realising their dreams of becoming parents,” Summer believes.
“I love it when patients return with a healthy baby for cuddles, after seeing them as a tiny embryo in the lab,” Kim agrees. “This makes every tough day worth it, knowing that so much joy is coming from it. I love speaking with patients and helping to guide them through the difficult decisions they need to make. I love working with the team as we all share common goals, and that is to see each patient journey end in success.”
“I truly value the fact that we can guide patients through their treatment and to be able to explain to them the latest scientific developments that we implement, but I also quite appreciate the fact that each day in the lab is different, each patient is a new opportunity of success,” Francisca adds. “Furthermore, in order to be an Embryologist, one has to have a broad spectrum of knowledge, from Biology to Law, Mathematics to Pharmaceutical Sciences, etc. and personally I enjoy this side of my job.”

 Making these changes in the run-up to egg freezing has no downside and could have a significant positive impact. We have supported several women who have had unsuccessful egg freezing rounds and collected no eggs towards outcomes they were really happy with. They have made changes to their diet and lifestyle and have been able to collect viable eggs on their next round.
Making these changes in the run-up to egg freezing has no downside and could have a significant positive impact. We have supported several women who have had unsuccessful egg freezing rounds and collected no eggs towards outcomes they were really happy with. They have made changes to their diet and lifestyle and have been able to collect viable eggs on their next round.

